Emerging food regimes: THE KETOGENIC DIET
The ketogenic diet (KD) or even ketonic as it can be found in literature, is a diet with very little carbohydrate intake. More than a diet, due to its potential and its application in certain pathophysiological conditions, a real metabolic treatment could be defined.
The ketogenic diet unlike other diets, in fact stands out for its effect that manifests itself not so much for the nutrients taken by the person but for the nutrients completely eliminated from the diet. It is a diet of deprivation that if scrupulously followed, succeeds in guaranteeing its effects in different ways and on different systems and systems of the human organism.
Very commonly we hear of a ketogenic diet in discussions centered on weight loss, but the experts know very well that this is a real family of diets that have as their only common aspect, that of being strongly hypoglycidal; in addition to the parameter of practically absent carbohydrates, they can also be hypolipidic or hyperlipidic, leaving the protein component which remains mostly on the intake as per the guidelines unchanged.
What is it?
Born in the last century in America, ketogenic diets have seen the beginnings in neurology due to the extraordinary power of being a real therapy for resistant drug epilepsy and then also appearing as a valid approach to the obese patient, type II diabetic, dyslipidemic and currently being studied for areas of medicine ranging from gynecology to oncology.
Starting therefore from a normoproteic contribution, to guarantee a state of ketosis to the patient, the development of a ketogenic food plan foresees a maximum intake of carbohydrates <50g / day and of lipids between 30g / day up to almost all of the caloric intake in case of application in neurology.
The state of ketosis is by no means a foregone conclusion, but very weak in a healthy body. Thanks to the glycidic depletion, the organism subjected to this regimen draws in the first days of treatment, hepatic and muscular glycogen, after which, it looks for an alternative fuel: the ketone bodies *. Ketosis in a context of energy need and in the total absence of exogenous and endogenous carbohydrates, becomes the only way to derive energy from a lipid matrix that can be endogenous, therefore adipocytic triglycerides or exogenous from alimentary fat.
It does not present itself as an easy diet, especially as it is limiting from a social point of view, restricting food choices to certain vegetables and protein second courses (meat or fish). As an alternative to fresh foods there are commercially available protein powders or substitute foods that mimic glycidic food despite being mostly protein and fatty foods.
Who can do it?
The ketogenic diet is a diet that promises great efficacy but also hides some pitfalls from a healthy point of view, so much so that it must always be carried out under specialized control. The national and international guidelines have provided not only indications (1, 2) but also essential contraindications, where the ketogenic diet must be avoided:
- diabetes type I
- acute myocardial heart attack
- kidney failure
- liver failure
- pregnancy
- breast feeding
- psychiatric illnesses
* VLCKD ketogenic diets (Very-Low-Calorie Ketogenic Diet) mainly use the state of physiological ketosis to obtain energy. Ketone bodies (acetone, acetate acetate and beta-hydroxy butyrate) are produced in the liver from fatty acids and then released into the circulation to provide an alternative energy substrate to the body’s sugars.
What role do lipids play?
Due to the technical and nutritional composition of this particular dietary approach, attention is usually paid above all to avoiding carbohydrate in its entirety and to take proteins from high biological value sources. Due to the great importance that they have an important look, it is necessary to address it to lipids, hypothesizing to evaluate the quality given to the patient on a ketogenic diet, both in the case of the obese patient who takes a few grams, but especially for the neurological patient who finds 90% of the calories represented by lipids alone.
In detail, in humans, polyunsaturated fatty acids (PUFAs) must be introduced with the diet because there are no enzymes to synthesize them. For the omega 6 (ω-6) and the omega 3 (ω-3) the contribution of at least the two founders is necessary, linoleic acid (LA, C18: 2) and alpha linolenic acid (ALA, C18 : 3), but their endogenous conversion in longer chain ω-6 and ω-3 fats is not very efficient and is reduced with age, with smoking and based on genetics.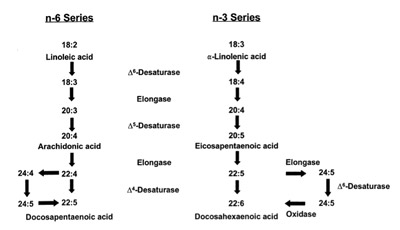
Figure 1: biosynthetic pathways of polyunsaturated fatty acids ω-6 and ω-3 with desaturation, elongation and beta oxidation. Observe the sharing of the same enzymes Δ-6 and Δ-5 oxidase (3).
Animal models agree that caloric restriction can have positive effects on health (healthspan) and on lifespan (lifespan). In some studies (4) it appears that caloric restriction, although having general positive effects, alters the hepatic lipidoma and therefore the profile of cellular fatty acids. It could therefore be hypothesized that even ketogenic regimens, as “mimed-fasting” or otherwise restrictive from the energy point of view, can induce similar changes.
Unfortunately, the scientific literature lacks exhaustive studies that evaluate which changes induce KD in the lipid composition of cell membranes, but it is clear that they occur, as indicated in a 2004 publication in the journal Prostaglandins Leukot Essent Fatty Acids (5):
“The KD causes a switch to ketogenesis that is coordinated with an array of changes in cellular lipid, amino acid, carbohydrate and inflammatory pathways.”
Given that the 20 carbon atoms (eicosanoids) PUFAs in cell membranes are, among other things, precursors of signal molecules (prostaglandins, thromboxanes, leukotrienes, etc.), it would be interesting that the scientific world would investigate what changes take place in this important cellular sector.
The SIE consensus statement (1) prescribes supplementation with 1 g / day of ω-3. The value appears generic because it does not specify the type or types of fatty acids to be chosen within this category and the primary objective is to avoid running into deficiencies of this nutrient. Compared to the various products on the market, it is not known at all that fish oil supplements have a decidedly lower omega 3 content than the weight in grams of the cell; the rest of the weight is saturated or monounsaturated fatty acids.
In ketogenic diets that use foods it is almost impossible not to exceed with protein foods containing saturated fats or ω-6 (red or sliced meats). An evaluation of the basal condition and an ad hoc integration would be desirable to avoid negatively affecting the membrane balance which, in overweight or obese subjects or with other comorbidities, is assumed to be already altered from the start.
What about lipoproteins?
Scientific studies show not yet conclusive results on plasma lipoproteins, also due to the lack of long-term trials and to the difference between ketogenic diets in comparison. Some studies report an increase in HDL cholesterol, of high density LDL cholesterol while a reduction in small and dense LDL, consider the most atherogenic.
Supplementation with well-balanced ω-3 would be a further element to ensure a balance of plasma lipoproteins, a necessary (but not sufficient) condition for cardiovascular health.
On the other hand, a reduction in triglyceridemia may be noted in people using KDs to reduce weight excesses. The reduction of triglycerides is also observed in the liver of subjects with non-alcoholic hepatic steatosis (NAFLD) who undergo KD.
Bibliography:
- Caprio M., et al. Consensus statement. Very-low-calorie ketogenic diet (VLCKD) in the management of metabolic diseases: systematic review and consensus statement from the Italian Society of Endocrinology (SIE). Journal of Endocrinological Investigation. 2019.
- Pezzana A., et al. The ketogenic diet. Foundation of the Italian Association of Dietetics and Clinical Nutrition. 2014.
- Lauritzen L, et al. The essentiality of long chain n-3 fatty acids in relation to the development and function of the brain and retina. Progress in Lipid Research 40 (2001) 1-94.
- Jove M., et al. Caloric restriction reveals a metabolomic and lipidomic signature in liver of male mice. Aging Cell (2014) 13.
- Cullingford TE. The ketogenic diet; fatty acids, fatty acid-activated receptors and neurological disorders. Prostaglandins Leukot Essent Fatty Acids. 2004
- Volek, J.S., et al. Modification of lipoproteins by very low-carbohydrate diets. J. Nutr. 2005
Articolo a cura di:
Piero Labate –PhD, Nutritionist
Francesco Bonucci – MSc, Nutritionist
The diet advise, written in the article, are not intended to be a substitute for a personal nutrition plan and should be adapted to specific cases
Photo: 123RF Archivio Fotografico: 76269417 ©Nadia Borovenko /123rf.com | 46989142 ©Phonlawat Chaicheevinlikit /123rf.com